Enhancing drug-safety
monitoring


A third project, SPaRCS, aims to strengthen pharmacovigilance systems and the clinical trials oversight capacity of national regulatory authorities in Eswatini, Namibia, South Africa and Zimbabwe. Having mapped the pharmacovigilance systems in the four countries and identified areas of strength, gaps and opportunities for learning, the project team developed a programme of activities to share expertise and build capacity. This included a webinar on pharmacovigilance and clinical trials oversight in sub-Saharan Africa in the era of COVID-19, held in May 2021.
During 2021, these activities focused primarily on pharmacovigilance, with clinical trials oversight a priority for 2022. The team has developed a training presentation on adverse drug reaction reporting, targeted at community health workers. This has been piloted in South Africa and will be adapted for use in the other countries.

The third PROFORMA five-day pharmacovigilance training course on ‘Signal Detection and Management’ was held online in January–February 2021. A total of 48 individuals working at national medicine regulatory authorities, universities, neglected tropical diseases programmes and immunisation programmes, healthcare professionals and pharmacists from Ethiopia, Kenya, Rwanda and Tanzania participated in training.
The goal of the PROFORMA project is to improve pharmacovigilance infrastructure, post-marketing surveillance systems and clinical trial regulatory capacity in Ethiopia, Kenya, Rwanda and Tanzania. The project conducted a baseline assessment of the pharmacovigilance systems and infrastructure in each country to identify capacity-building priorities and developed associated national roadmaps. Based on these findings, medicines regulatory authorities in each country have developed and begun to implement national pharmacovigilance plans.
Activities in 2021 focused on the strengthening of pharmacovigilance programmes, based on the national roadmaps. In addition, in each of the four countries, academic, national medicine regulatory authorities and public health programmes conducted joint active cohort surveillance studies of mass drug administration and vaccination campaigns.
In terms of training, 12 individuals are working towards postgraduate qualifications under the PROFORMA umbrella (seven PhDs and five master’s students). In addition, an undergraduate pharmacovigilance curriculum (short course), a postgraduate pharmacoepidemiology and pharmacovigilance curriculum (master’s programme), and pharmacovigilance E-learning module for healthcare professionals have been developed and launched.
PROFORMA and PAVIA also jointly sponsored a symposium, ‘Equity in safety: improving pharmacovigilance of drugs and vaccines in Africa’, at the Tenth EDCTP Forum in October 2021. The symposium provided an opportunity to share the lessons learned from the two projects, and how they can be applied to COVID-19 vaccine safety surveillance.
Together with the EDCTP-funded PROFORMA project (see below), PAVIA is exploring the possibility of extending its remit to COVID-19 vaccination. In April 2021 the project organised a webinar on COVID-19 vaccine safety surveillance, involving project and regional partners including the WHO Regional Office for Africa, the African Vaccine Regulatory Forum (AVAREF) and the African Union Development Agency/New Partnership for Africa’s Development (AUDA-NEPAD).
The PAVIA project, for example, is developing a model for strengthening of pharmacovigilance systems through enhanced cross-sectoral collaboration, focusing on four countries – Eswatini, Ethiopia, Nigeria and Tanzania. The project has carried out landscape analyses of pharmacovigilance systems in each country and developed country-specific roadmaps for development of national pharmacovigilance capacity. In September 2021, the consortium published a guidance document, ‘Effective Implementation of a Pharmacovigilance Policy in Resource Limited Settings’ and is finalising a complementary guide to funding and financial models for sustainability of pharmacovigilance programmes.
In December 2021, the Eswatini national pharmacovigilance policy and implementation framework was formally launched at an event attended by key officials from the Ministry of Health, other government departments, and a range of national and regional stakeholders. The Principal Secretary of the Ministry of Health for Eswatini and the Honourable Minister of Commerce both acknowledged the support of the PAVIA team and other international stakeholders in the development of the policy.
In Tanzania, the PAVIA team has been supporting the development of an electronic reporting tool (aDSM) for reporting of adverse reactions associated with the use of TB medicines, work led by the Tanzania Medicines and Medical Devices Authority (TMDA). A multi-stakeholder meeting was held in July 2021 to finalise the tool, which is available on the TMDA website and as an Android app.
In parallel with the introduction of new TB drugs and treatment regimens for multidrug-resistant TB, Ethiopia has introduced a new aDSM system. Led by the Ethiopian Food and Drug Administration (EFDA), PAVIA supported the introduction of this new system at a range of training events in 2021. In addition, in June 2021 PAVIA contributed to a two-day inaugural meeting of a Causality Assessment Committee, which will investigate adverse drug reactions received via aDSM.
PAVIA also organised a range of other training events during the year, including introductory pharmacovigilance workshops for 140 health care workers in Tanzania, with a particular focus on TB treatments and use of electronic tools for reporting of adverse drug reactions. In addition, the third PAVIA session was held in June 2021, focusing on developing the capacity of national medicines regulatory authorities, with input from PAVIA project partners, the European Medicines Agency (EMA) and the Ghana Food and Drugs Authority (FDA).
scroll down
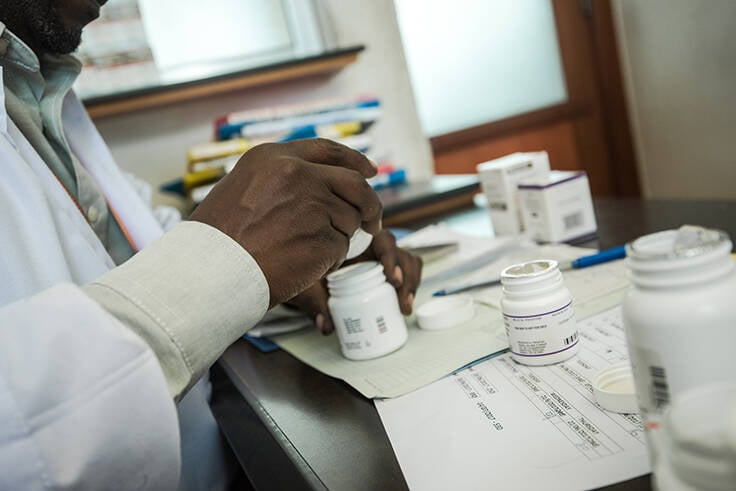
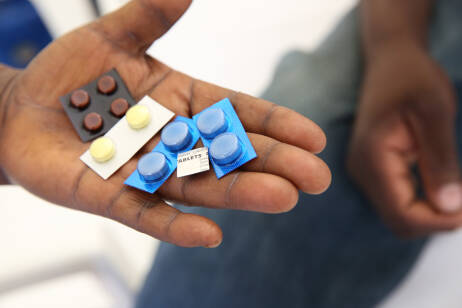
As new interventions are introduced across sub-Saharan Africa, it is important that they are monitored to identify and respond to any potential safety issues and to ensure public confidence in drug safety. EDCTP capacity building funding has included several collaborative projects focused on building national pharmacovigilance capabilities.
EDCTP projects have been promoting cross-sectoral and international collaborations to build national pharmacovigilance capacity in multiple sub-Saharan African countries.

Building capacity for drug safety monitoring
Ethiopian researchers investigating MDR-TB serious adverse events.
Pharmacovigilance training at the Raleigh Fitkin Memorial Hospital in Eswatini,
Project: PAVIA project: Pharmacovigilance Africa
Project lead: Professor Frank Cobelens, Stichting Amsterdam Institute for Global Health and Development, The Netherlands
Countries involved: Eswatini, Ethiopia, Italy, The Netherlands, Nigeria, Tanzania
Year funded: 2018
EDCTP funding: €3 M
Grant agreement: CSA2016S-1627
Project website: www.pavia-project.net
Professor Frank Cobelens
(The Netherlands)

What comes next for the project?
Frank Cobelens: In its final project year, PAVIA will wrap up with a number of key activities aimed at learning from the project and sustaining its achievements. These include a final assessment of pharmacovigilance capacity and performance in the four project countries, the creation of a blueprint for use in other sub-Saharan African countries that captures the lessons learned from the PAVIA project, transitioning of the e-learning courses developed as part of the bended learning onto an open-access platform to ensure its sustainability, and the publication of models for sustainable financing of pharmacovigilance activities in the African context.
What progress was made in 2021 toward the short-term and long-term project’s objectives?
Frank Cobelens: Eswatini developed and formally launched its first national pharmacovigilance policy and implemented it, helped by the policy guidance. PAVIA contributed to strengthening collaborations between regulatory authorities/ pharmacovigilance centres and public health programmes, including immunisation programmes, around safety surveillance of COVID-19 vaccines, for which the project provided training and organised a webinar attended by professionals from several other African countries.
We conducted two online train-the-trainer courses for the PAVIA blended learning programme, which includes e-learning on pharmacovigilance for healthcare staff involved in the treatment of multidrug-resistant TB (MDR-TB) and for general healthcare workers. Overall, we saw a continued increase in adverse event reporting for new drugs and regimens for MDR-TB treatment in three of the four project countries and increased analysis of those reports.
In 2021, the PAVIA Consortium published the guidance document ‘Effective Implementation of a Pharmacovigilance Policy in Resource Limited Settings’. How can this guide help countries implementing national pharmacovigilance (PV) policy? How is the consortium leveraging African development initiatives to assist in the uptake of PV roadmaps and guidance documents by national governments to inform domestic PV strengthening and implementation frameworks?
Frank Cobelens: In many African countries a major impediment to effective pharmacovigilance for poverty-related diseases, as well as for other medicinal products, is a lack of a functional regulatory framework, and of clear roles and responsibilities for stakeholders towards ensuring the safety of medicines. It is therefore key not only to develop national pharmacovigilance policies, but also to make sure that they are effectively implemented.
The guidance document describes the steps that need to be taken to that end, such as a formal launch of the policy, communication with the media, securing funding, planning research, and addressing the roles and responsibilities of stakeholders. Such stakeholders include ministries of health, regulatory authorities, public health programmes, and health delivery and professional organisations. The guide was put into practice in implementing pharmacovigilance policies in Nigeria and Eswatini, and may help other countries to plan implementation of their own (new) policies.
scroll down
Project Q&A